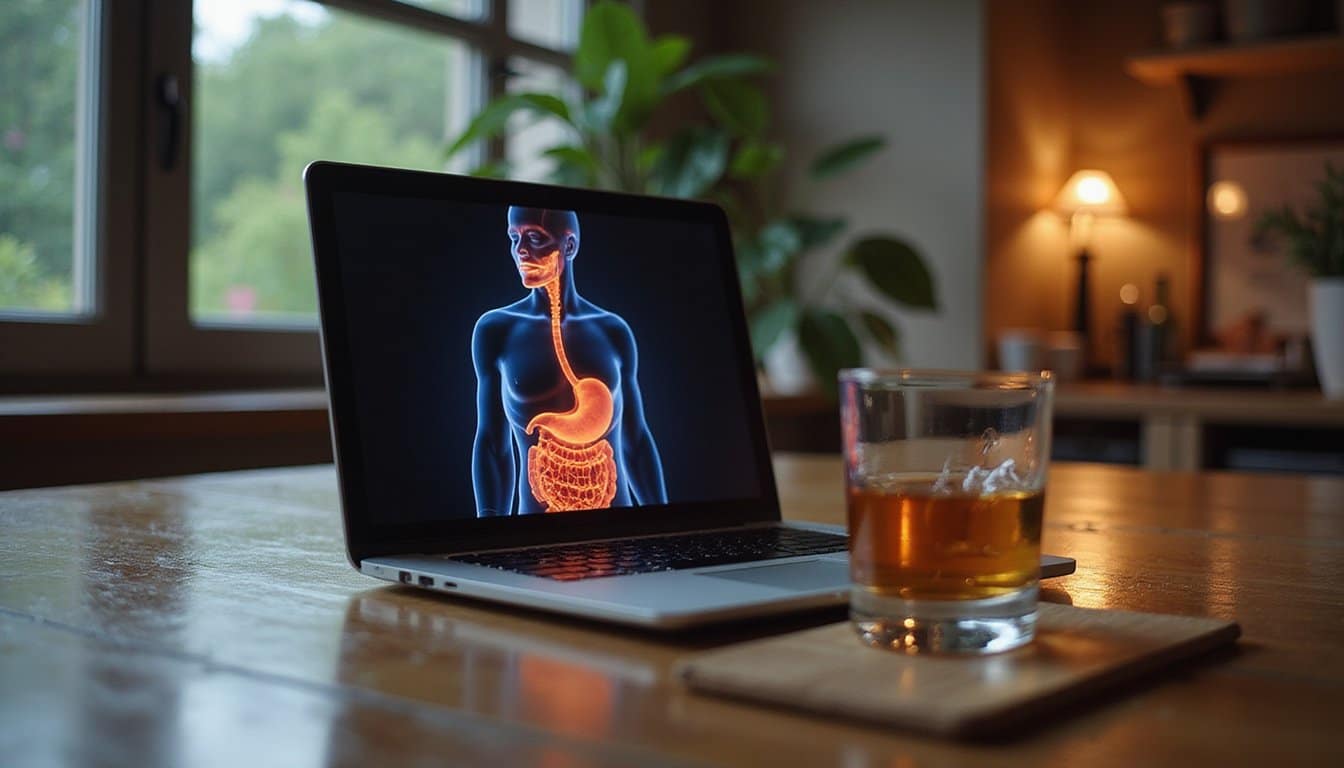
Does Alcohol Affect Gut Health? Startling Facts You Must Know
Find out how alcohol begins destroying your gut’s beneficial bacteria from your very first
Medically reviewed by Health Care Professional Robert Gerchalk, April 2025
Some medications may be used under medical supervision to manage symptoms of alcoholism, reduce alcohol cravings, or support recovery.
Disclaimer: Some medications (like Gabapentin, Seroquel, Hydroxyzine, Lorazepam, and Methadone) appear in both lists because they help with withdrawal but can be dangerous when combined with alcohol. They’re only safe after alcohol use has stopped, under medical supervision.
Always consult a qualified healthcare practitioner before starting any new medication, and take medications prescribed to you only as directed. Call us to connect with resources that can help you learn more or talk to your doctor.
Help reduce alcohol cravings or create negative reactions to alcohol.
Primarily used for opioid use disorder but sometimes involved in co-occurring substance treatment.
May help with anxiety, mood stabilization, and withdrawal symptoms.
Used to manage withdrawal symptoms like elevated heart rate and blood pressure.
Used off-label to help with anxiety, sleep, or nausea during withdrawal.
Support brain and nerve health, often depleted by chronic alcohol use.
Yes. Many common drugs that do not require a prescription, like acetaminophen (Tylenol), ibuprofen, and antihistamines, can interact with alcohol, increasing the risk of liver damage, drowsiness, or stomach bleeding.
Call your doctor or pharmacist right away, especially if you feel dizzy, confused, extremely drowsy, or unwell. If it’s an emergency, call 911 or seek medical attention immediately.
Mixing alcohol and marijuana can increase the effects of both, leading to stronger impairment, dizziness, nausea, or panic. It can also make it harder to judge how intoxicated you are, increasing the risk of accidents or overdose-like symptoms (sometimes called “greening out”). It’s generally safer to avoid using them together.
Yes. Even natural products like St. John’s Wort, kava, valerian root, and CBD can interact with alcohol, often by increasing sedation, dizziness, or liver strain. Just because something is “natural” doesn’t mean it’s safe to mix with alcohol. Always check with a healthcare provider.
Alcohol has the power to severely impact your life, but you also have the power to break free from your addiction. Call us today and connect with someone who can refer you to an appropriate treatment program near you.

Getting a better understanding of the detox process can vastly improve the chances of a successful recovery for you or a loved one.
If you or someone you love is dealing with an alcohol use disorder, this information should serve as an overview of the treatment options available.

Discovering AlcoholAwareness.org marked a pivotal moment in my journey to sobriety; their insights and support brought a new level of clarity and hope, profoundly impacting my life.
Debbie S.
The resources and guidance from AlcoholAwareness.org helped me understand my alcoholism and empowered me to embrace a fulfilling and sober lifestyle.
Sam T.
Thanks to AlcoholAwareness.org, I navigated the complexities of recovery with their practical advice and empathetic support, leading me to a stronger, sober future.
Jason B.
Explore research and expert perspectives that can help you make informed decisions about alcohol to support your health and your future.

Find out how alcohol begins destroying your gut’s beneficial bacteria from your very first

Struggling with alcohol’s grip on your relationships reveals painful truths, but the powerful coping

Here’s what alcohol really does to your eyes, and the permanent damage it causes
Fill out our confidential form whenever you’re ready.
Your information stays private, and our team will respond with compassion, clarity, and the support you deserve.
Fill out our confidential form whenever you’re ready.
Your information stays private, and our team will respond with compassion, clarity, and the support you deserve.