Face rash while detoxing from alcohol can occur as the immune system becomes overactive during withdrawal. When drinking stops, inflammatory cytokines such as TNF-α and IL-6 may surge, while mast cells release histamine, leading to vasodilation, facial flushing, and hives. At the same time, alcohol’s diuretic effects often leave the skin’s moisture barrier depleted, increasing sensitivity and irritation. Individuals with the ALDH2 genetic mutation are particularly susceptible to pronounced facial redness due to impaired acetaldehyde metabolism. Understanding how these factors interact helps explain why facial rashes develop during detox and guides more targeted symptom relief.
How Alcohol Withdrawal Triggers Immune System Hyperactivation
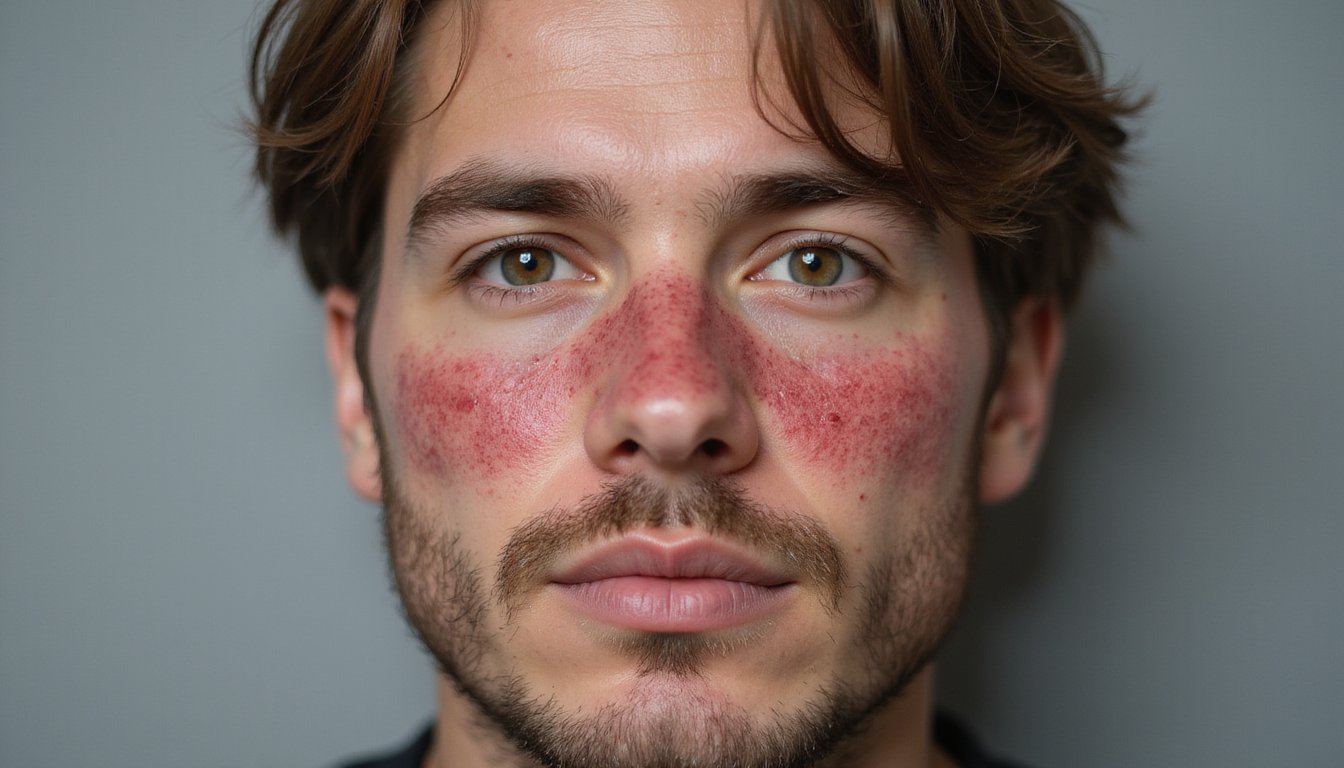
When you stop drinking after prolonged alcohol use, your immune system doesn’t simply return to normal, it goes into overdrive. Your body releases amplified levels of TNFα, IL-1β, and IL-6, triggering widespread immune cell activation. This cytokine mediated skin inflammation can manifest visibly, particularly on your face.
During withdrawal, NFκB activation drives pro-inflammatory cytokine expression throughout your body. Research shows GFAP increases 16-fold and CD11b 18-fold in chronic alcohol exposure, indicating significant glial cell activation. These inflammatory signals don’t stay confined to your brain, they affect peripheral tissues, including your skin. Chronic alcohol consumption also disrupts the blood-brain barrier, allowing greater influx of immune cells and cytokines that can spread throughout the body.
Your neurovascular skin reactivity heightens as stress hormones remain enhanced in key brain regions. This persistent inflammatory state, combined with compromised immune regulation, creates conditions where facial rashes commonly develop during detoxification. The downregulation of GABA receptor function during chronic alcohol use means your nervous system loses its ability to properly regulate inflammatory responses, further exacerbating skin reactions during withdrawal. Studies have shown that elevated MCP-1 levels in individuals with alcohol use disorder are positively associated with peripheral markers of alcohol-induced inflammation, contributing to systemic immune dysregulation that affects the skin.
The Role of Histamine Release in Facial Redness and Hives
As your body processes alcohol and enters withdrawal, histamine release becomes a primary driver of facial skin reactions. Alcohol and acetaldehyde directly trigger mast cells to release histamine while simultaneously inhibiting diamine oxidase, the enzyme responsible for breaking histamine down. This dual mechanism creates heightened histamine levels that act on H1 and H2 receptors in your facial blood vessels.
The resulting effects include:
- Vasodilation causing visible flushing across your cheeks, nose, and forehead
- Urticaria presenting as raised, itchy wheals from vascular leakage
- Pruritus triggered by histamine binding to sensory nerve endings
If you have cross reactivity with food allergies or existing atopic dermatitis risk factors, you’re more susceptible to pronounced histamine responses during detox. Rebound mast cell activity can amplify these reactions beyond baseline drinking periods. Individuals with a genetic mutation in ALDH2, commonly seen in those of East Asian descent, may experience more severe facial redness due to inefficient alcohol metabolism and acetaldehyde accumulation. These facial rashes typically arise within 12 to 48 hours after the last drink, making early monitoring essential during the initial detox phase. In cases of chronic liver disease, increased production of bile salts can accumulate under the skin and further stimulate itchiness alongside these histamine-driven reactions.
Dehydration and Skin Barrier Breakdown During Detox

When you stop drinking, alcohol’s diuretic effects leave your skin depleted of essential moisture, compromising the protective barrier that shields your face from irritants. This dehydration impairs your skin’s ability to retain water and produce ceramides, creating dry, flaky patches that become vulnerable to inflammation and rash development. Acetaldehyde, the toxic byproduct your body produces when metabolizing alcohol, can also contribute to skin irritation and heightened sensitivity during this vulnerable period. Alcohol’s inflammatory properties can also trigger broken capillaries on the nose and cheeks, adding to facial redness and uneven skin tone. The compromised state of your skin during detox also increases susceptibility to bacterial and fungal infections, which can manifest as rashes on the face. If you scratch these irritated areas, you’ll further damage the weakened barrier, intensifying facial redness and prolonging your skin’s recovery during detox.
Alcohol’s Diuretic Effects
Alcohol acts as a potent diuretic by suppressing vasopressin, the hormone that signals your kidneys to retain water. This triggers rapid fluid loss, with research showing increased urine output within four hours of drinking. Your body prioritizes hydration for essential organs, drawing moisture away from your skin first.
During detox, you’ll experience these compounding effects:
- Electrolyte depletion disrupts cellular hydration balance
- Sweat gland dysfunction impairs your skin’s natural cooling and moisture regulation
- Sebum quality changes create an oily surface masking deeper dehydration
Higher alcohol content beverages accelerate this dehydration cycle. As your body loses water and salt, your skin barrier weakens, allowing ceramide function to deteriorate. This compromised barrier lets moisture escape while permitting environmental irritants entry, setting the stage for rash development. Additionally, your liver requires extra water to metabolize alcohol’s toxins, further depleting the fluid reserves your skin desperately needs during recovery. Chronic alcohol consumption also impairs nutrient absorption, depriving your skin of essential vitamins and minerals needed to maintain its protective barrier and repair damaged tissue. Drinking water between alcoholic beverages may help decrease dehydration risk and minimize the severity of these skin barrier disruptions during the detox period.
Impaired Skin Moisture Retention
Your skin’s protective barrier takes a significant hit during alcohol detox, creating conditions ripe for facial rashes. Chronic alcohol exposure depletes essential stratum corneum lipids, ceramides, cholesterol, and fatty acids, resulting in lipid barrier deficiency that accelerates moisture loss. This damage increases transepidermal water loss, leaving your face dry, tight, and vulnerable to irritants.
Compromised epidermal water retention compounds these effects. When your epidermis lacks adequate hydration, cells contract, desquamation slows, and microscopic cracks develop. These fissures allow allergens and microbes to penetrate more easily, triggering inflammation that presents as rash-like roughness or erythema. Alcohol also dissolves protective lipids in the stratum corneum, further weakening your skin’s front line of defense against environmental toxins. The resulting disruption contributes to accelerated skin aging through glycation and free radical damage, which further compromises the skin’s ability to heal.
The good news: once you stop drinking, barrier repair begins within weeks. Hydration typically starts normalizing within 24, 72 hours of abstinence, with early improvements in skin softness and reduced dryness-related irritation. As your body continues to heal, stronger circulation delivers more oxygen and nutrients to skin cells, supporting faster recovery of the damaged barrier.
Scratching Worsens Facial Rash
Beyond moisture loss, the mechanical act of scratching creates a separate pathway for rash worsening during alcohol detox. When you scratch itchy facial skin, you trigger scratch response dynamics that perpetuate inflammation. Your nails break the already compromised epidermal layer, allowing irritants deeper access and increasing infection risk.
The inflammatory mediator involvement compounds this damage through three key mechanisms:
- Scratching releases histamines, which intensify your itch sensation and create a self-perpetuating cycle.
- Your immune system overreacts to micro-trauma during withdrawal, amplifying redness and swelling.
- Sleep disturbances common in detox lead to unconscious nighttime scratching that worsens lesions.
Dehydration makes your skin crack more easily under scratching pressure. Combined with nutrient deficiencies that slow healing, this mechanical trauma considerably prolongs facial rash duration during detox. The good news is that some of these damaging effects, including blotchiness and dryness, may improve with time when you stop drinking and follow proper treatment protocols.
Nutritional Deficiencies That Cause Skin Problems in Recovery

Your body’s nutritional stores become severely depleted during alcohol abuse, and these deficiencies directly affect your skin’s ability to heal and maintain itself. Vitamin C deficiency can cause scurvy, which manifests as purpura and petechiae on your face, while zinc deficiency produces raised, crusting lesions around your eyes, nose, and mouth. Additionally, anemia from folate deficiency impairs oxygen delivery to healing tissues, slowing your recovery from detox-related skin damage.
Vitamin C and Scurvy
Because heavy alcohol consumption severely impairs your body’s ability to absorb and retain vitamin C, scurvy, once considered a historical disease, remains a real concern during alcohol detox. Research shows 42% of alcohol use disorder patients in ICU settings have severe vitamin C deficiency. Without adequate vitamin C, your body can’t maintain proper collagen production, which directly affects tissue repair and skin integrity.
During recovery, watch for these warning signs:
- Petechiae and perifollicular hemorrhages appearing on your skin
- Corkscrew hairs and follicular hyperkeratosis
- Easy bruising and poor wound healing
Your treatment team may recommend high-dose oral vitamin C supplementation alongside thiamine to correct deficiencies safely. This approach supports liver detoxification, reduces oxidative stress, and helps restore your skin’s health without adverse effects.
Zinc Deficiency Effects
How drastically does zinc deficiency affect your skin during alcohol detox? If you’ve struggled with chronic alcohol use, you’re at high risk, up to 90% of people with alcohol use disorder have inadequate zinc intake due to poor diet and malabsorption.
Zinc deficiency produces a distinctive rash pattern. You’ll notice dry, scaly, sharply edged patches around your mouth, eyes, and on your hands and feet. These lesions can progress to crusted, pustular plaques that mimic eczema or seborrheic dermatitis.
The consequences extend beyond appearance. Inadequate topical zinc and systemic depletion cause slow skin cell turnover, weakening your skin barrier and delaying wound healing. Your damaged skin becomes vulnerable to secondary bacterial and fungal infections. You may also develop cheilitis, glossitis, and nail changes alongside facial dermatitis.
Anemia Worsens Healing
When anemia develops during alcohol detox, your skin’s ability to heal slows dramatically because oxygen delivery to damaged tissue drops. Reduced tissue oxygenation impairs keratinocyte and fibroblast function, resulting in delayed collagen deposition and weakened wound repair. Chronic alcohol use causes anemia through multiple mechanisms:
- Folate and B12 deficiency produces megaloblastic anemia, disrupting DNA synthesis in rapidly dividing skin cells.
- Iron malabsorption compromises hemoglobin production and enzymatic systems essential for cellular energy.
- Bone marrow suppression reduces red blood cell output, magnifying oxygen deficits during early abstinence.
These hematologic changes mean your facial rash takes longer to resolve. Even after you stop drinking, red blood cell recovery lags because cells live approximately 120 days. Nutritional rehabilitation with folate, B12, and iron repletion gradually restores healing capacity.
Pre-Existing Skin Conditions That Flare During Alcohol Cessation
Although alcohol cessation benefits your overall health, it can trigger significant flare-ups if you have pre-existing skin conditions. During withdrawal, your body experiences aggravated skin sensitivity and an immunity dysregulation response as it recalibrates without alcohol’s suppressive effects.
If you have eczema or dermatitis, expect intensified itchiness and redness as stress hormones surge. Psoriasis plaques may worsen, particularly on your hands and face, due to proinflammatory cytokine activation. Urticaria sufferers often notice more prominent facial hives from heightened histamine release.
Seborrheic dermatitis can intensify because nutritional deficiencies impair your skin’s resilience. Contact dermatitis becomes more reactive as dehydration compromises your skin barrier. Your immune system’s rebound sensitivity amplifies these conditions temporarily. Consult your dermatologist if flare-ups become severe or treatment-resistant during your detox process.
Liver Function and Its Impact on Facial Skin During Withdrawal
Your liver serves as your body’s primary detoxification organ, and its function directly affects your facial skin’s appearance during alcohol withdrawal. When alcohol damages your liver, toxin buildup triggers skin manifestations including acne, redness, and irritation. Hormonal dysregulation from impaired liver function increases oestrogen levels, causing spider telangiectases and palmar erythema.
Your liver’s healing journey during alcohol withdrawal reveals itself through clearer, healthier facial skin.
During withdrawal, your liver begins healing, producing measurable changes:
- Heightened AST and ALT enzymes normalize within 4-8 weeks, signaling reduced inflammation
- Bilirubin processing improves, diminishing jaundice’s yellow skin discoloration
- Hematological changes stabilize as detoxification efficiency increases
You’ll notice clearer, more hydrated skin as your liver eliminates toxins effectively. The CDC confirms alcohol abstinence restores skin health disrupted by consumption. Early enzyme reduction within 7-14 days marks your healing’s start.
Stress Hormones and Their Effect on Detox-Related Rashes
Beyond liver function, stress hormones play a significant role in detox-related skin manifestations. When you stop drinking, your body enters an extreme stress state, triggering heightened catecholamine activity. These stress hormones relax blood vessel walls, raising your core temperature and causing visible flushing across your face, neck, and chest.
Simultaneously, cortisol driven inflammation amplifies your immune response. Increased cortisol levels increase inflammatory cytokines, leading to skin swelling, dermatitis, and urticaria. Research shows 70% of rosacea patients experience alcohol-triggered flare-ups through these stress pathways.
Your autonomic nervous system’s overactivity compounds these effects, contributing to persistent rashes. Treatment approaches include stress management techniques like meditation, which reduce skin inflammation during detox. Additionally, nutritional support with B-vitamins and proper hydration help mitigate hormone-related dermatological symptoms throughout your recovery process.
When to Seek Medical Attention for Facial Rash During Detox
Most facial rashes during alcohol detox resolve with basic supportive care, but certain warning signs require immediate medical attention. You should monitor rash severity thresholds closely, as progression beyond mild irritation often indicates a more serious underlying condition.
Seek emergency care if you experience:
- Swelling of your face, tongue, or throat, which signals potential anaphylaxis requiring immediate intervention
- Non-blanching petechial rashes suggesting vitamin C deficiency or vascular involvement
- Rash accompanied by severe withdrawal symptoms like tremors, vomiting, or dehydration
Your healthcare provider will perform a concurrent medical history evaluation to identify contributing factors such as liver disease, thyroid dysfunction, or nutritional deficiencies. Persistent rashes lasting beyond the acute detox phase, worsening despite hydration, or burning sensations warrant professional assessment to rule out inflammatory conditions requiring targeted treatment.
Why Facial Rashes Can Appear During Alcohol Detox
Noticing a sudden rash or redness on your face while detoxing from alcohol can feel alarming, especially when your body is already going through so many changes. As alcohol leaves the system, the body begins adjusting its immune response and circulation, which can sometimes trigger temporary skin reactions during early recovery. If you or someone you care about is experiencing uncomfortable detox symptoms, an Inpatient alcohol treatment center can connect you with trusted treatment centers and medical professionals who know how to manage withdrawal safely. Call +1-855-955-0771 today and let us help you take that first step toward healing, completely confidential and ready to help.
Frequently Asked Questions
How Long Does a Facial Rash Typically Last During Alcohol Detox?
Your facial rash typically resolves within 3, 7 days as acute withdrawal symptoms subside, though rash duration variability depends on several factors. If you’ve experienced prolonged heavy drinking or have contributing medical conditions like liver impairment, nutritional deficiencies, or pre-existing skin disorders such as rosacea, your symptoms may persist longer, up to two weeks. If your rash worsens or continues beyond this timeframe, you should seek medical evaluation to rule out underlying causes.
Can Over-The-Counter Antihistamines Safely Treat Detox-Related Facial Rashes?
You can safely use non-sedating antihistamines like cetirizine or loratadine for histamine-related hives and itching during detox. However, they won’t address all rash causes. If antihistamines don’t provide relief, you may need topical steroids for localized inflammation or oral corticosteroids for more severe reactions, both require medical guidance. Avoid first-generation antihistamines due to sedation risks. If you experience facial swelling, breathing difficulty, or blistering, seek immediate medical care.
Will the Facial Rash Return if Someone Relapses After Detox?
Yes, your facial rash will likely return if you relapse after detox. When you resume drinking, alcohol metabolites trigger immediate flushing and histamine release, causing rashes within hours. Your skin sensitivity changes during recovery make you more vulnerable to severe reactions. Additionally, underlying skin condition flare ups, like eczema or dermatitis, intensify with relapse stress. The rash may match or exceed your original detox symptoms, especially if your skin barrier hasn’t fully healed.
Does the Severity of Alcohol Addiction Affect Facial Rash Likelihood?
Yes, your addiction severity directly influences facial rash likelihood during detox. Higher alcohol withdrawal severity correlates with greater liver damage, nutritional deficiencies, and immune dysregulation, all increasing your skin’s vulnerability. More intense withdrawal triggers stronger autonomic responses, worsening flushing and rash probability. Your detox program duration may need extension if you’ve experienced prolonged heavy use, as cumulative physiological damage requires additional time for proper hydration, nutritional support, and medical monitoring to address skin complications effectively.
Can Certain Skincare Products Worsen Facial Rashes During Alcohol Withdrawal?
Yes, certain skincare products can considerably worsen facial rashes during alcohol withdrawal. Your increased skin sensitivity makes you more vulnerable to potential irritants in products, including sulfates, parabens, fragrances, and alcohol-based formulations. These ingredients penetrate your compromised skin barrier more easily, triggering contact dermatitis or intensifying existing inflammation. You’ll want to switch to fragrance-free, gentle formulations and avoid harsh exfoliants until your skin stabilizes. Consult your dermatologist for personalized recommendations.

